Cells of bone and Bone remodeling/turnover (Note)
Bone is a specialized form of connective tissue that consists of cells and intercellular material.
Osteoblasts, osteocytes and osteoclasts make up the cells of the bone, while the inter-cellular material is made of organic and inorganic material.
By dry weight, bone comprises of 33% organic matrix, with 28% representing type I collagen, and non-collagenous proteins like bone sialoprotein, osteocalcin, osteopontin, osteonectin and proteoglycans making up 5%. The organic matrix is mineralized by hydroxyapatite (inorganic material), which comprises the rest of the 67% of bone by dry weight.
BONE CELLS
Bone cells are of two types, one being osteogenic or bone forming and the other being osteoclastic or bone resorbing.
Cells of the bone are osteoblasts, osteocytes and osteoclasts.
Osteoblast
Osteoblasts, mesenchymal in origin, are plump cuboidal cells that line the outer surfaces of bone.
When inactive, osteoblasts lining the bone are flat and are called bone lining cells.
Osteoblasts help lay down the organic matrix called osteoid and are rich in an enzyme called alkaline phosphatase. Alkaline phosphatase is hypothesized to help in initiation and growth of mineral crystals.
Osteocyte
During bone formation when the organic matrix is laid down by osteoblasts, they often get buried within the lamellae and are housed in small cavities called lacunae.
Osteoblasts housed in lacunae are called osteocytes and they have delicate cytoplasmic processes radiating out that are housed in micro canals called canaliculi.
These canaliculi are interconnecting and help in osteocytes contact adjacent osteocytes as well as the osteoblasts lining the bone surface. Overall, it helps in maintaining nutrition and vitality of the bone.
Osteocytes also act as mechanosensors, transducing signals to the bone helping in bone remodeling and maintaining the integrity of the bone.
Osteoclast
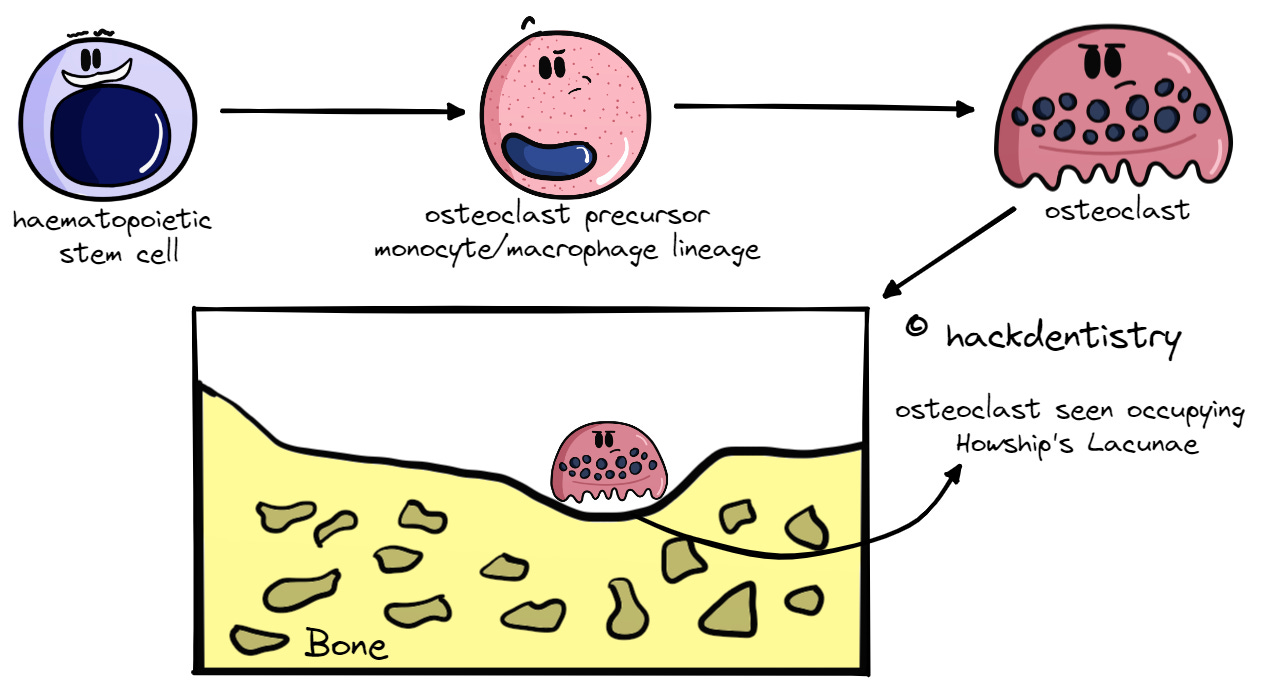
Osteoclasts are haematopoietic in origin and are derived from the monocyte/macrophage lineage of cells.
They are large multinucleated giant cells having around 15-20 nuclei, whose function is to resorb bone.
They play a very important role in bone remodeling and are characterized by the presence of an enzyme called tartrate resistant acid phosphatase (TRAP). Osteoclasts can be seen occupying shallow depressions called “Howship’s lacunae” during active resorption of bone.
BONE REMODELING
The structural integrity of bone is maintained by removal of old or damaged bone by osteoclasts and subsequent replacement with new bone by osteoblasts.
This process is called bone remodeling and it also helps release of calcium and phosphate from bone thus helping their metabolism and maintaining mineral homeostasis.
The process of bone remodeling can either be targeted or non-targeted.
Targetted and Non-Targetted Bone Remodeling
- Targeted remodeling is aimed at a particular site in the bone where there is damage or insult. The damaged bone is resorbed and is then replaced with new bone.
- Non-targeted remodeling however is not confined to any particular site in the bone and is a systemically controlled process. It refers to the remodeling controlled by hormones like parathormone, thyroxine or estrogen. Non-targeted remodeling could help release calcium and phosphate from bone and thus help their regulation and maintain homeostasis.The process of remodeling happens within anatomic sites called Basic Multicellular Units (BMU) or bone remodeling units (BRU).
The BMU comprises of osteocytes, osteoblasts, lining cells (mature osteoblasts), osteoclasts and a vascular supply.
STEPS IN BONE REMODELING
Bone remodeling is a continuous and a dynamic process, which for the sake of understanding could be separated into 5 key events that occur within a course of 120-200 days.
These events or steps in the remodeling process are
Activation
Resorption
Reversal
Formation and
Termination
(Scroll further down for the illustration of the steps in Bone Remodeling)
Activation
Osteocytes are key cells that play a major role in bone remodeling. They act as mechanosensors, transducing signals to the bone helping in bone remodeling.
Daily activities could cause mechanical strain to the bone inducing micro damage and osteocyte apoptosis. Also there may be signals to the bone from hormones for maintaining mineral homeostasis.
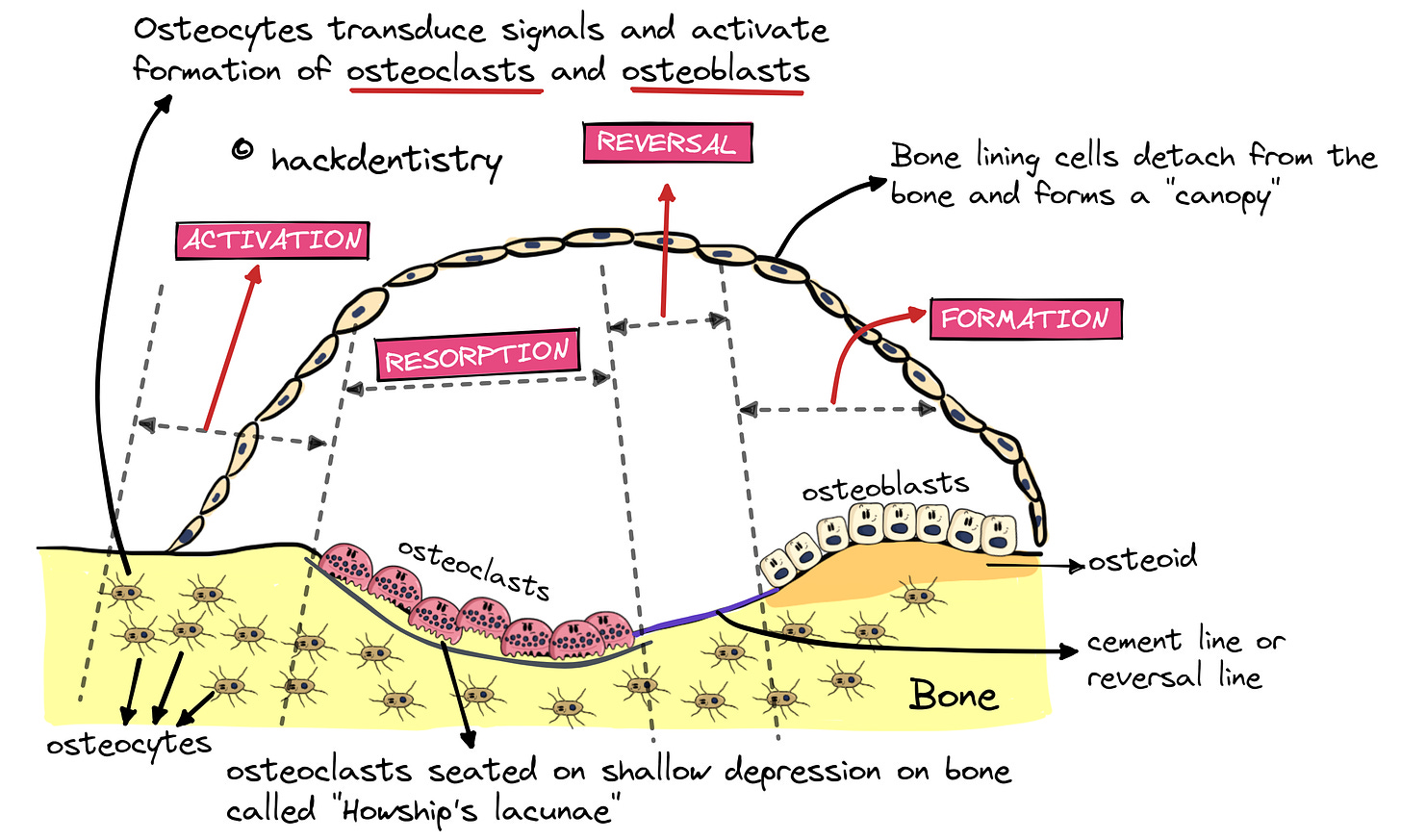
Either way, osteocytes transduce signals that activate formation of osteoclasts and osteoblasts.
Simultaneously, the bone lining cells covering the target area of bone to be remodeled raises or detaches to form a canopy exposing the underlying bone.
Resorption
Monocytes from the blood vessels migrate to the site of remodeling and differentiate to multinucleated osteoclasts in response to signaling factors like macrophage colony stimulating factor (M-CSF) and RANK ligand (RANKL) secreted by the bone lining cells.
Once fully differentiated, osteoclasts attach to the bone, form a sealing zone and resorb bone (refer the note and video - “Bone resorption process by osteoclasts.“).
On resorption, the bone develops a shallow trench or depression called the Howship’s lacunae. In fact, under the microscope, active osteoclasts are always found resorbing bone, housed in Howship’s lacunae.
This phase is terminated by osteoclast apoptosis. This curtails excess resorption from happening.
Note
Now though all events happening in bone remodeling are the same for both cortical and cancellous bones, there is a difference in the way bone is resorbed.
- In cancellous bones, osteoclasts resorb and form a trench or depression on the surface of the bone which is then filled with new bone.
- In cortical bones however, the osteoclasts resorb by forming what is called a “cutting cone” and bores a tunnel into the bone.
- Blood vessels grow into this tunnel and bone is subsequently formed around the blood vessel. This leads to the formation of an osteon otherwise called a Haversian system.Reversal
After bone resorption, osteoclasts detach from the bone and undergo apoptosis.
Macrophages remove the collagen debris from the area of resorption and make way for osteoblasts to lay down new bone.
Mesenchymal stem cells, once in the site of remodeling, differentiate into osteoblasts and secrete a layer of non-collagenous proteins on the bone surface.
This non-collagenous protein layer termed cement line or reversal line acts as a cohesive, between the old bone and the new bone to be deposited.
Formation
New bone deposited happens in two stages – formation of organic matrix or osteoid followed by mineralization of the matrix by hydroxyapatite.
The areas in the tunnel in cortical bones that are being filled by new bone are called filling cones.
Termination
Once new bone is formed, osteoblasts could end up having multiple fates.
They could
undergo apoptosis,
become inactive bone lining cells or
become buried in the newly formed bone as osteocytes.
HIGHLIGHTS - VIVA & ENTRANCE EXAM PERSPECTIVE
Osteoblasts, osteocytes and osteoclasts make up the cells of the bone, while the inter-cellular material is made of organic and inorganic material.
Bone cells are of two types, one being osteogenic or bone forming and the other being osteoclastic or bone resorbing.
When inactive, osteoblasts lining the bone are flat and are called bone lining cells.
Osteoblasts help lay down the organic matrix called osteoid.
During bone formation when the organic matrix is laid down by osteoblasts, they often get buried within the lamellae and are housed in small cavities called lacunae.
Osteoblasts housed in lacunae are called osteocytes and they have delicate cytoplasmic processes radiating out that are housed in micro canals called canaliculi.
Osteoclasts play a very important role in bone remodeling and are characterized by the presence of an enzyme called tartrate resistant acid phosphatase (TRAP). They can be seen occupying shallow depressions called “Howship’s lacunae” during active resorption of bone.
The process of remodeling happens within anatomic sites called Basic Multicellular Units (BMU) or bone remodeling units (BRU).
Events or steps in the remodeling process are a) Activation, b) Resorption, c) Reversal, d) Formation and e) Termination.
Osteocytes are key cells that play a major role in bone remodeling. They act as mechanosensors, transducing signals to the bone helping in bone remodeling.
This non-collagenous protein layer termed cement line or reversal line acts as a cohesive, between the old bone and the new bone to be deposited.
REFERENCES AND FURTHER READING
Kenkre JS, Bassett J. The bone remodelling cycle. Ann Clin Biochem. 2018 May;55(3):308-327.
Matsumoto, Mariza & Biguetti, Claudia & Fonseca, Angélica & Saraiva, Patrícia. (2016). Bone Tissue Healing Dynamics: From Damage to Reconstruction. Journal of Molecular Signaling Updates. 1. 33-40.
Eriksen EF. Cellular mechanisms of bone remodeling. Rev Endocr Metab Disord. 2010;11(4):219-27.
Nanci A. Tencate’s Oral Histology. Development, Structure and Function. 8th ed. Elsevier; 2013.
Young B, Woodford P, O’Dowd G. Wheater’s Functional Histology. A Text and Colour Atlas. 6th ed. Elsevier Churchill Livingstone; 2014.
Kumar GS. Orban’s Oral Histology and Embryology.13th ed. Elsevier; 2011.
Lindhe J, Lang NK, Karring T. Clinical periodontology and implant dentistry. 5th ed. Blackwell Munksgaard;2008.