Oral Mucosa - An Introduction (Note & Video)
This section would give you an introduction of what the oral mucosa is and how it is structured. Also remember that, knowledge and awareness of what the oral epithelium is and how it is structured is a prerequisite for understanding the histopathology of various diseases occurring in the oral cavity (which you would learn in Oral Pathology).
COMPONENTS OF THE ORAL MUCOSA
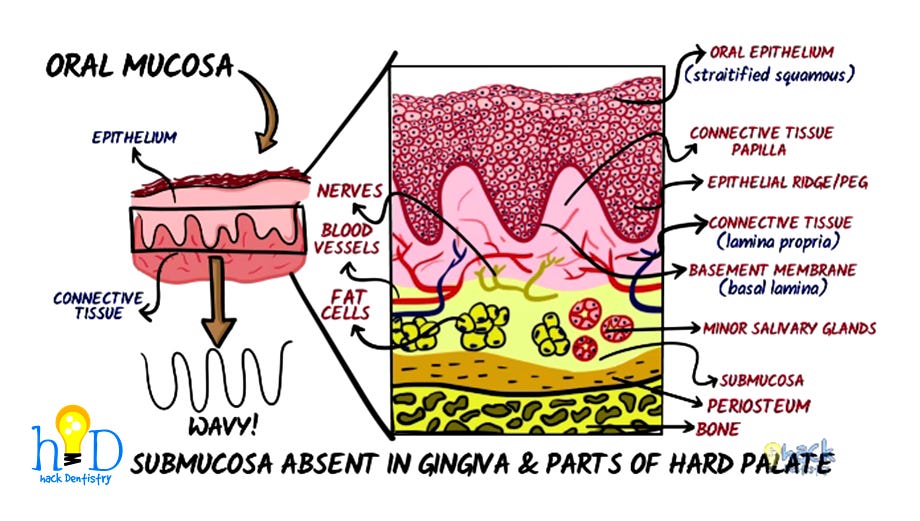
The two main components of the oral mucosa are 1) the oral epithelium called stratified squamous epithelium and 2) the underlying connective tissue, also called lamina propria.
WHY IS THE ORAL EPITHELIUM TERMED "STRATIFIED SQUAMOUS"?
- The oral epithelium is described as being a "stratified squamous epithelium".
- The term "stratified" refers to the oral epithelium being stacked in layers. Epithelium having 2 or more layers of cells are said to be "stratified" (see Figure 2 & 3).
- The term "squamous" was derived from cells being compared to the scales of a fish. In general, squamous cells are flat with their height being lesser than their width.
- Interestingly (as you will learn subsequently), the oral epithelium is described as being squamous based on the shape of the cells on the upper surface (which are flat). The lower most layer of cells (in the stratified squamous epithelium) called the basal cells, are cuboidal or low columnar in shape.The epithelium and connective tissue interface is wavy and undulating with the connective tissue papillae interdigitating with the epithelial ridges or pegs.
The junction between the epithelium and connective tissue is called the basement membrane and is ultra- structurally referred to as the basal lamina.
Below the lamina propria is another layer of connective tissue called the submucosa consisting of minor salivary glands, fatty tissue, major blood vessels and nerves which attaches the overlying tissues to the underlying bone or muscle.
WHAT IS CONNECTIVE TISSUE?
- In the oral mucosa, connective tissue (lamina propria) comprises the tissue below the oral epithelium.
- The submucosa beneath the lamina propria, is also a form of loose connective tissue.
- Connective tissue, in general, gives mechanical support and nutrition to the epithelium.
- They account for the elasticity and the tensile strength of the oral mucosa.TYPES OF STRATIFIED SQUAMOUS EPITHELIUM
Stratified squamous epithelium in the oral cavity, can be keratinized and non-keratinized.
The “masticatory mucosa“ is composed of keratinized epithelium and the “lining mucosa“ is composed of non-keratinized epithelium.
The dorsal surface of the tongue forms the “specialized mucosa“ due to the presence of taste buds and other sensory functions.
Keratinized epithelium/Masticatory mucosa
The gingiva and the hard palate constitute the masticatory mucosa (keratinized epithelium).
Since they are subject to frequent abrasion during mastication, they have a layer of keratin (see Figure 2) to make them tough and bear the forces of mastication.
Non-Keratinized epithelium/Lining mucosa
The rest of the oral cavity (apart from gingiva, hard palate and dorsum of tongue) - lips, cheeks, floor of the mouth, ventral surface of tongue, constitute the lining mucosa and are devoid of a keratin layer (see Figure 3).
LAYERS OF STRATIFIED SQUAMOUS EPITHELIUM
Keratinized epithelium/Masticatory mucosa
The keratinized epithelium consists of 4 layers or strata namely
the basal layer or stratum basale,
the prickle cell/spinous layer or stratum spinosum,
the granular layer or stratum granulosum and
the corneal/keratinized layer or stratum corneum
Non-keratinized epithelium/Lining mucosa
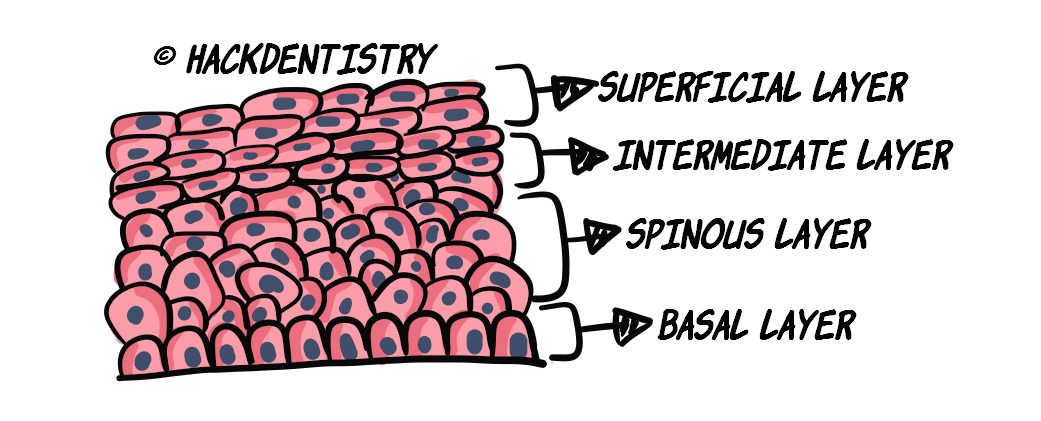
The non-keratinized epithelium consists of 4 (or 3) layers or strata namely
the basal layer or stratum basale,
the prickle cell/spinous layer or stratum spinosum,
the intermediate layer or stratum intermedium and
the superficial layer or stratum superficiale
Some prefer to avoid the use of the term prickle cell or spinous layer and consider only 3 layers in the non-keratinized epithelium.
ORAL EPITHELIUM - PROLIFERATION
All cells in the body have a limited life span, after which they die by a process called “apoptosis” or programmed cell death. So how then, does the oral epithelium maintain its integrity?
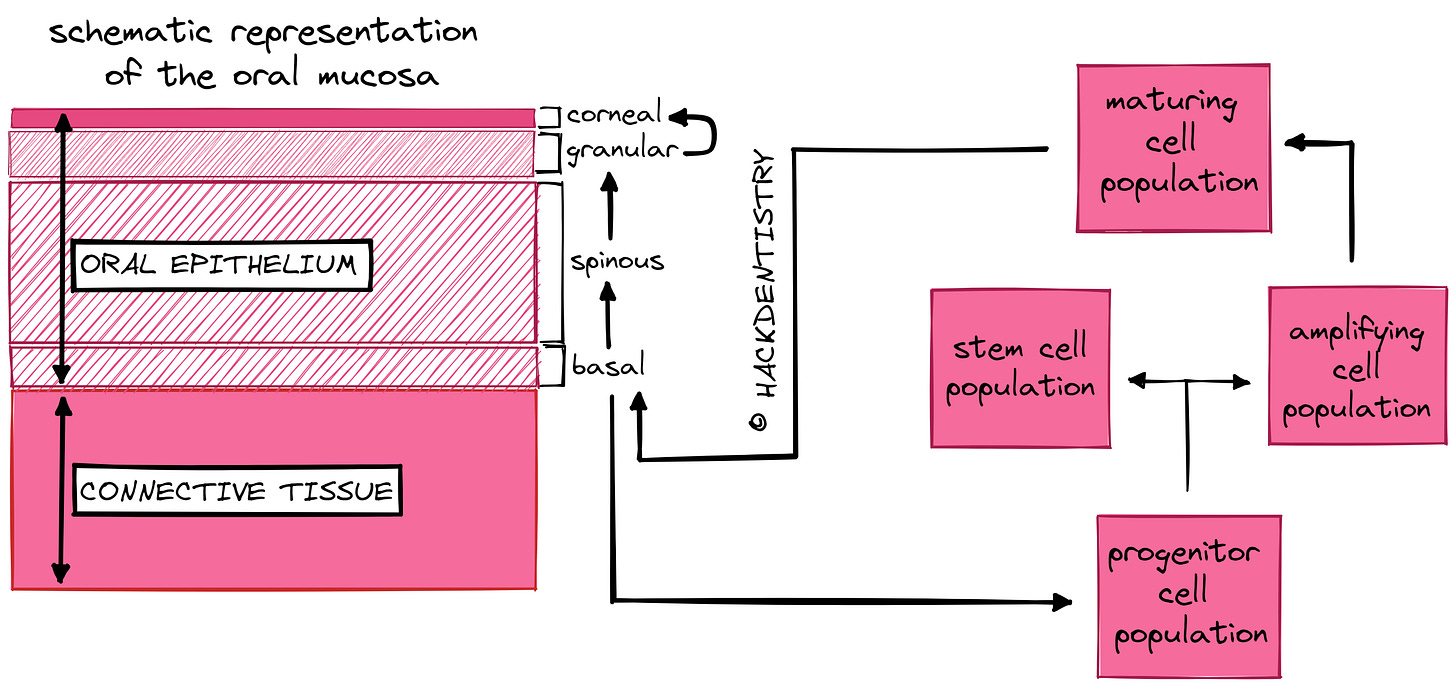
Studies show that the there are two population of cells in the basal layer -> a) progenitor cells and b) maturing cells.
Progenitor cells keep producing new cells for proliferation and maturing cells mature and differentiate into the the various cells in the different layers.
A (basal) cell matures and differentiates to become a spinous cell -> which further differentiates to become a granular cell and -> then loses its organelles and nucleus to become a corneal cell densely packed with keratin. The corneal cell is finally shed.
This way, cells in the lower layers divide and produce new cells, which in turn undergo maturation as they keep moving up layers and replace cells that are shed.
Progenitor cells further, have 2 sub-population of cells called a) stem cells and b) amplifying cells.
Stem cells are the cells that have the potential to produce new cells for further proliferation and amplifying cells increase the maturing cell population (that mature and differentiate).
HIGHLIGHTS - VIVA & ENTRANCE EXAM PERSPECTIVE
The two main components of the oral mucosa are the oral epithelium called stratified squamous epithelium and the underlying connective tissue, also called lamina propria.
The term “stratified“ refers to the oral epithelium being stacked in layers. Epithelium having 2 or more layers of cells are said to be “stratified” (see Figure 2 & 3).
The term “squamous“ was derived from cells being compared to the scales of a fish. In general, squamous cells are flat with their height being lesser than their width.
The epithelium and connective tissue interface is wavy and undulating with the connective tissue papillae interdigitating with the epithelial ridges or pegs.
The junction between the epithelium and connective tissue is called the basement membrane and is ultra- structurally referred to as the basal lamina.
The “masticatory mucosa“ is composed of keratinized epithelium and the “lining mucosa“ is composed of non-keratinized epithelium.
The dorsal surface of the tongue forms the “specialized mucosa“ due to the presence of taste buds and other sensory functions.
The keratinized epithelium consists of 4 layers or strata namely -> stratum basale, spinosum, granulosum and corneum.
The non-keratinized epithelium consists of 4 (or 3) layers or strata namely -> stratum basale, spinosum, intermedium and superficiale.
Some prefer to avoid the use of the term prickle cell or spinous layer and consider only 3 layers in the non-keratinized epithelium.
REFERENCES AND FURTHER READING
Berkovitz BKB, Hollan GR, Moxham BJ. Oral Anatomy, Histology and Embryology. 4th ed. Mosby Elsevier; 2009.
Nanci A. Tencate’s Oral Histology. Development, Structure and Function. 8th ed. Elsevier; 2013.
Kumar GS. Orban’s Oral Histology and Embryology.13th ed. Elsevier; 2011.
Avery JK. Oral development and Histology. 3rd ed. Thieme Medical Publishers; 2002.
Young B, Woodford P, O’Dowd G. Wheater’s Functional Histology, A Text and Colour Atlas. 6th ed. Elsevier Churchill Livingstone; 2014.